So, I’ve always been guilty of not rotating my pump sites enough, in fact you could call me downright resistant. I guess when I find something I like, I just want to stick with it and after all, I do ask my Endo about it occasionally and he always replies in his usual fashion “All looks good Julie”.

And this pic is only my 7th month…yikes!
For years, I used to use my belly for my Omnipod and rotate through about 6-8 sites but last year, during my pregnancy, I had an enormous belly and a lot of discomfort with my pump, so I started relying on only two sites.
Since then (it’s been 13 months!), I guess I just got lazy, or caught up with putting life ahead of routine diabetes management…we’ve all been there right? Frankly, I still have 28lbs of baby weight to lose and the old sites (which were largely around my waistband) just aren’t comfortable anymore.
Well, I started noticing that it looked my insulin needs were increasing?! It didn’t make sense: I was breastfeeding, not overweight (technically), active, hadn’t changed my eating habits, other medications, etc. WTH?!
It finally dawned on me that maybe my poor old sites were just worn out. I Googled it and came across lipohypertrophy and then got scared out of my pants by doing an Image Search for it (fyi, don’t click on this Image Search unless you’re fully ready for the unsettling consequences). Enough said…site rotation here I come!
Now, I don’t have any signs of lipohypertrophy yet but when I was pregnant, my insulin needs tripled and it makes sense that my insulin absorption rates for those belly sites might have taken a toll.
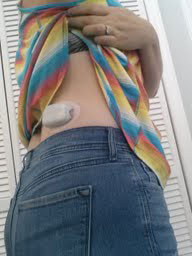
I’m currently a proud wearer of a back Omnipod…day two 😉 It has it’s issues and will take some getting used to (especially when I try to carry a backpack)…but my sugars have been much lower, while everything else has stayed pretty much the same (same insulin rates, same diet and activity, same morning and afternoon coffee, same evening glass of wine…you get the picture). So far this experiment is a success, Phew!
Stay tuned for more pod placement experimentation…